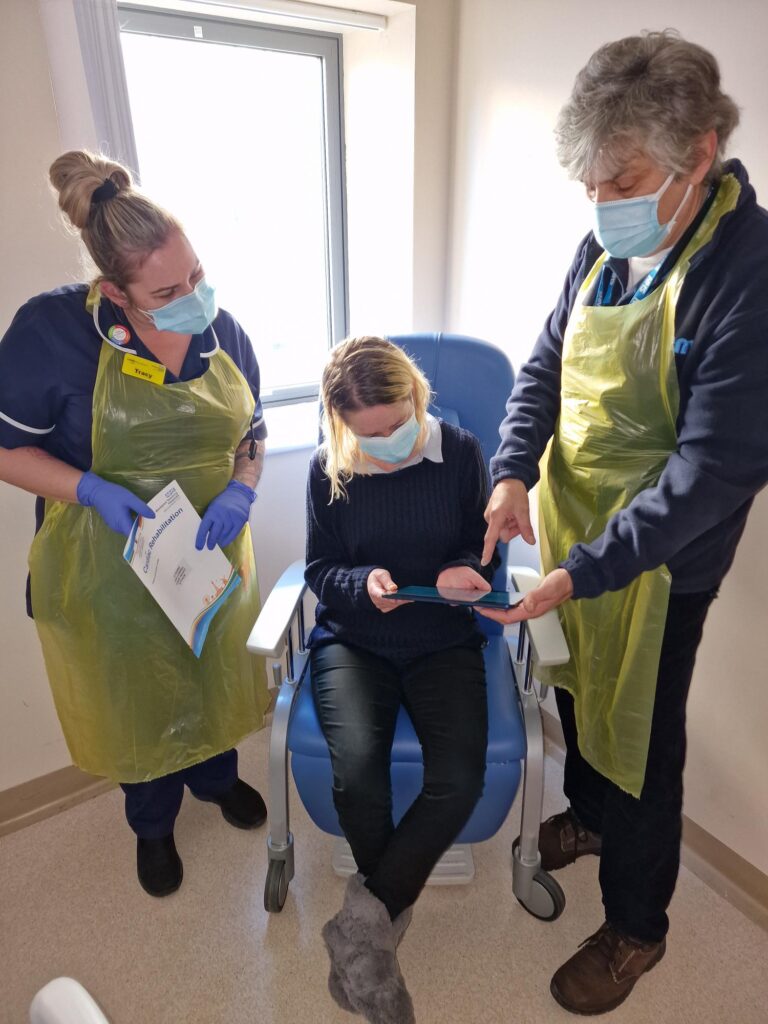
 A new technology solution provided by the Lancashire Cardiac Centre at Blackpool Teaching Hospitals is allowing post-operative heart attack patients to return home from hospital sooner.
A new technology solution provided by the Lancashire Cardiac Centre at Blackpool Teaching Hospitals is allowing post-operative heart attack patients to return home from hospital sooner.
The Early Discharge Pathway is being led by the Trust’s Consultant Cardiologist Dr Tawiq Choudhury and has been hailed a success by patients who following discharge receive digital monitoring using the latest technology, virtual platforms and frequent follow-ups.
The pathway has been adopted in collaboration with Barts Health NHS Trust, London where this pathway is now routinely used. Use of the virtual platform and remote monitoring allows closer follow-up of patients than would be the case with the previous model of care where patients are kept in hospital for longer and then followed up at a much later timepoint than with the remote monitoring pathway.
Dr Choudhury has been working with the remote monitoring team to establish the pathway at Blackpool and to date has recruited 25 patients with excellent feedback.
“Patients can have access to specialist support whilst continuing their recovery in their own homes, which we know has improved outcomes,” said Rachel Haworth, Project Lead at Blackpool Teaching Hospitals. “Covid-19 has created enormous pressure on the healthcare system. As well as the obvious benefits for the patient, this service will also improve bed efficiency without compromising patient safety or quality of care.
“The data feeding through is showing positive results, with all patients that accessed the service, remained out of hospital in the first seven days of discharge. Patients have reported ‘having access to a digital platform has really enhanced their care.’”
Sarah Fishwick and Helen Davies, Lead Cardiac Specialist Nurses at Blackpool Teaching Hospitals said: “The Early Hospital Discharge Pathway for STEMI patients has been a really positive step in patient care, using interactive technology to help monitor patients at home following an early discharge, who would have otherwise been an inpatient for longer.
“The benefits for the patients include being at home in their own surroundings to recover whilst being closely monitored by a team. The patient then gets a virtual clinic follow-up phone call/videocall at week 1, week 4, and week 12 in which the home observations are reviewed, medication compliance and up titration of medications is offered to maximise the medication potential.
“Any further investigations are followed up and there is a collaborative care effect involving Cardiac rehab. The feedback we have received within the virtual clinic has been really positive from patients, who have embraced the collaborative care and involvement in their own recovery.”
Susan Ashmore, Coronary Care Unit (CCU) Ward Manager said: “The early hospital discharge pathway has been well received by patients and Coronary Care Unit staff. It has enabled those patients who meet the criteria to be discharged home sooner and freed CCU beds up earlier for other emergency admissions.”
 Natalie Marsden from Fylde Coast Medical Services (FCMS) said: “The Early Discharge Pathway means more patients can be cared for at home, where most prefer to be. Working with this excellent team is demonstrating great results. Patients can recover at home sooner and be more engaged in their own care, their feedback speaks for itself. This new way of working releases hospital bed capacity making it another example of real-world transformation.”
Natalie Marsden from Fylde Coast Medical Services (FCMS) said: “The Early Discharge Pathway means more patients can be cared for at home, where most prefer to be. Working with this excellent team is demonstrating great results. Patients can recover at home sooner and be more engaged in their own care, their feedback speaks for itself. This new way of working releases hospital bed capacity making it another example of real-world transformation.”
How The Early Discharge Pathway Works
After a patient has undergone an emergency heart procedure at the Lancashire Cardiac Centre, their treating consultant will identify in the labs whether they are eligible for the Early Discharge service. This is then followed up by the nursing team on the ward who will offer this service to the patient and refer them to service provider FCMS so that they can ‘onboard’ the patient by their bedside on the very same day. Once the patient is confident using the BP machine and Docobo device, they are discharged from the hospital and are able to go home just 24 hours after their procedure.
FCMS have a combination of clinicians including ACPs, Practice Nurses, Assistant Practitioners and HCAs who closely monitor the patient for seven days following their hospital discharge via the Docobo system. These clinicians review answers to daily questions such as how they are feeling and whether they are experiencing any specific symptoms.
If nurses have any concerns, they engage with the patient over the phone and escalate to either the GP or hospital if necessary. The patient can also speak to one of a specialised tech team or clinicians at any time for support via the helpline number they are provided with on the day of their discharge.
After seven days a video call appointment facilitated by the Docobo device will take place with the patient and their assigned Cardiac Specialist Nurse, ensuring no unnecessary trips to the hospital are required. Following this the patient is ‘offboarded’ – meaning they are no longer being monitored remotely.
Patients then have two more telehealth follow up appointments until eventually the process is complete and the patient will be off boarded, and the remote monitoring equipment is collected from their home.